News
Recent news and press releases of the Delaware Valley ACOFuture Trends to Watch for Value-Based Care
Dr. Mark Angelo, CEO and President and Joel Port, Senior Vice President of Business & Network Development share their thoughts on the Future Trends to Watch for Value-Based Care including:
- Increased Adoption By Health Care Providers
- Use of Advanced Analytics and Technology
- Social Drivers of Health and Health Equity
- Personalized Medicine, Patient-Centered Care, and Outcomes
How Main Line Health, Delaware Valley ACO Used Palliative Care to Cut Hospitalizations by 50%
How Main Line Health, Delaware Valley ACO Used Palliative Care to Cut Hospitalizations by 50%
The Delaware Valley Accountable Care Organization (ACO) has leveraged a comprehensive, community-based palliative care program developed by its partner Main Line Health to reduce costs of care by $9,000 per eligible patient.
Among Delaware Valley’s palliative care recipients, hospital admissions were 50% lower and emergency department visits fell by 35%, generating about $9,000 in savings per patient during the last 90 days of life, according to Beth Souder, the ACO’s vice president of clinical operations.
Delaware Valley ACO CEO Mark Angelo on the future of value-based care

Delaware Valley ACO CEO Mark Angelo on the future of value-based care
“What we’re doing is changing the paradigm of care,” Angelo said.
Read Mark’s projections for the future of value-based care in a recent interview on Healthcare Brew responding to the following questions:
- How would you describe your job to someone who doesn’t work in healthcare?
- What would you consider the most challenging part of your job?
- What healthcare trend are you most optimistic about, and why?
- Do you think the 2030 goal is feasible?
DVACO Presenting at the ACHE 2023 Congress on Healthcare Leadership
We are happy to announce that we will be presenting at the ACHE 2023 Congress on Healthcare Leadership! This event features an incredible group of leaders exploring practical solutions to the challenges we face in healthcare today.
Be sure to join us for our presentation Managing Value-Based ACO Performance Focusing on Network Performance and Health Equity Through Advanced Analytics on Wednesday, March 22nd from 3:15-4:15pm. Hope to see you at #ACHECongress! #ACO #POPULATIONHEALTH #VALUEBASEDCARE #DelawareValleyACO #MSSP
Check out the other presenters and sessions here: https://congress.ache.org/
DVACO Recognizes 2022 Healthcare Quality Week
DVACO Recognizes 2022 Healthcare Quality Week
Healthcare Quality Week is celebrated each year during the third week in October. The week is dedicated to acknowledging the progress made by healthcare quality professionals and the work they do to improve patient outcomes. This special time also allows for reflection on past successes, and preparation for the challenges and opportunities that lie ahead.
Each day, healthcare quality professionals focus on enhancing patient care and improving outcomes and value. They work in every area of healthcare. Healthcare quality roles include patient safety, regulation, accreditation, analytics, quality review, just to name a few.
At the center of the recognition is the acknowledgement of healthcare professionals who strive for a safe, quality patient experience throughout the industry. The week also focuses on education, quality activities and allows for sharing both tools and protocols, such as the free webinars offered by the National Association of Healthcare Quality (NAHQ) Free NAHQ webinars. All activities are designed to improve outcomes and provide the highest quality care possible.

DVACO Quality Improvement Team
Lauren Talley, Kim Burgess, Tina Sokolowski, Toni Arnold
Beth Souder, Emma Myers, Ginna Bodycot, Jeanette Flood
Payton Watts, Sherrie Eisman, Juli Gruber-May, Gina Gibson
Nancy Welsh, Vicki Vitacco Hansell, Terry Tull
Kyle Brown, Emmy Stup, Nhi Tran, Jennifer Pawlowski
(top to bottom, left to right)
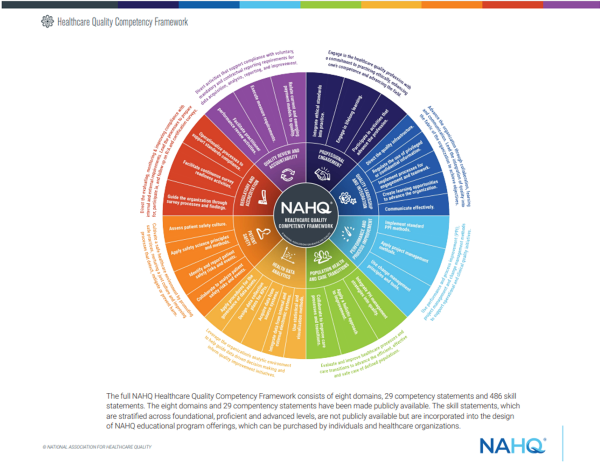
Since 1985, the National Association of Healthcare Quality (NAHQ) has been using Healthcare Quality Week to highlight the important role that healthcare quality professionals play in their organizations. NAHQ also provides the industry-standard framework for healthcare quality competencies that reduce variability of healthcare delivery, by offering a common vocabulary and toolset. NAHQ’s Healthcare Quality Competency Framework, shown below, articulates everything that must be present in a high-functioning quality program and offers career pathways for individuals to explore and is shown below.
Ginna Bodycot BSN, RN DVACO Director of Quality Improvement shared the following:
“At DVACO one of many ways Quality Improvement is carried out is through the work of the Quality Operations/Oversight Group which convenes each month to cooperatively drive quality efforts in the physician offices, hospitals, and outpatient facilities. Serving are representatives from DVACO and our partner organizations that represent quality, clinical, pharmacy, outreach, practice transformation, analytics, and contracting departments. This dynamic and dedicated Group generously share best practices, tools, identify solutions to barriers and celebrate big and little wins together associated with improved processes and care. It is the Healthcare Quality Competency Framework in action.”

DVACO Recognizes World Hospice and Palliative Care Day
DVACO Recognizes World Hospice and Palliative Care Day
Saturday, October 8th was World Hospice and Palliative Care Day- World Hospice and Palliative Care Day 2022 (thewhpca.org). According to The Worldwide Hospice and Palliative Care Alliance, it is estimated that each year 57 million people are in need of palliative care services worldwide with 25 million people at the end-of-life. The underutilization of these services results in 18 million people dying in unnecessary pain and distress each year. The Delaware Valley Accountable Care Organization’s (DVACO) mission is to accelerate high quality value-based care in the region.
Liz Todd, PT, DPT, DVACO Manager of Care Continuum, said the following:
See the links above for more information on World Hospice and Palliative Care Day; DVACO Care Coordination; and DVACO’s Preferred Hospice Network, respectively.
Mark Angelo, M.D. on Advancing Health Equity in Palliative and Hospice Care
Mark Angelo, M.D. on Advancing Health Equity in Palliative and Hospice Care
It was welcomed news when the Centers for Medicare and Medicaid (CMS) announced its commitment to promoting equity in health care as an essential tenet of improving the health care delivery system. At a July 19, 2022 forum sponsored by CMS through the Value Based Care Learning System, Mark Angelo, M.D., who serves as Chief Medical Officer of the Delaware Valley ACO, as well as its President and Chief Executive Officer, contributed to this aim by participating in a national panel on Advancing Health Equity in Palliative and Hospice Care.
Discussing the persistent disparities in care in the US healthcare system, Dr. Angelo, who is board certified in palliative medicine, observed the following: “We [may] experience a larger dependency on post-acute care in underrepresented minority population, because of all the social factors that surround [this] population…often [they] are diagnosed with later stage illness and may face inferior outcomes to treatment based on access to care.” The panelists concurred that systemic racism may also impact the rate at which minorities experience less than optimal treatment in hospital facilities and inequal access to home care.
Dr. Angelo identified challenges providers face in having crucial conversations with patients, stating, “Communications in end of life are super difficult. . . throw in disparities between the people having the communication . . .[such as] different levels of understanding [and] preconceived notions that each bring to the table.” The conversation among the panel pointed to a growing body of research in the field, indicating, for example, that such preconceived notions have been shown to lead to differences in medication prescription across ethnicities due to beliefs about pain tolerance or biases about the potential for abuse.
Discussing initiatives at DVACO, Dr. Angelo noted an internal DVACO study regarding access to Transcatheter Aortic Valve Replacements (TAVR) in historically underserved communities. (TAVR is a breakthrough treatment that uses a catheter to replace the aortic valve instead of breaking the chest open.) A review conducted by DVACO found that patients residing in more affluent, predominately White zip codes receive TAVRs much more frequently than patients with similar diagnoses who are Black and/or who do not reside in such areas. Dr. Angelo noted that DVACO is actively working with community cardiologists to promote awareness of the disparity and improve access for this life saving procedure.
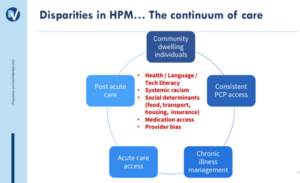
Figure 1. For more information on CMS Health Equity initiatives, visit CMS.gov or click here.
Main Line Health, Jefferson Health Announce New Equity Partner For Delaware Valley Accountable Care Organization
Main Line Health, Jefferson Health Announce New Equity Partner For Delaware Valley Accountable Care Organization
Philadelphia, Pa. (July 12, 2022)—Main Line Health and Jefferson Health, two of the region’s largest health systems, today announced Humana Inc., one of the nation’s leading health and well-being companies, will become an equity partner in the Delaware Valley Accountable Care Organization (DVACO). DVACO, first established as a joint venture between Main Line Health and Jefferson Health, supports more than 250,000 total patient lives across various government and commercial programs and is designed to provide personalized, proactive and affordable care for patients in a cost-effective and efficient delivery system.
“We established the DVACO to lead the way in improving health in our region by embracing and advancing value-based care. We are excited by the opportunity to add such a well-respected expert in managing population health—with a proven track record of success—to our partnership,” said John J. (Jack) Lynch, FACHE, president and CEO of Main Line Health. “This new agreement allows us to continue building on the foundation DVACO has created and bring even more support to our payer partners’ programs, physicians, care teams and, most importantly, patients.”
“We are excited about this new opportunity to improve the health of our region. DVACO’s mission is to accelerate the transformation to high quality value-based care, and by adding the expertise, experience and resources of the country’s leading Medicare Advantage programs, we can continue this important work, offer care teams more support and further enhance the experience and outcomes of the communities we serve,” said Dr. Bruce A. Meyer, president of Jefferson Health and senior executive vice president of Thomas Jefferson University.
The agreement with Humana will provide DVACO the ability to expand its services; more infrastructure to support performance in population-based and value-based contracting and enhance STAR quality ratings; as well as access to best-in-class tools, including advanced analytics and expertise in patient and physician engagement strategies and network management.
“We look forward to working alongside Main Line Health, Jefferson Health and all of DVACO’s partners to further expand the organization’s impact, particularly in caring for those who are seriously ill or medically vulnerable, while also addressing social determinants of health,” said Oraida Roman, vice president of Value-Based Strategies at Humana. “We are excited by the future we can create together and the positive impact we have in the lives of those we serve. It’s important for Humana to provide the support and resources that help patients and providers transition from fee-for-service to value-based care models because we know value-based care can not only improve health outcomes but also strengthen the healthcare system.”
Dr. Mark Angelo, interim president and CEO of DVACO, stated “Our goal at DVACO has always been to lead the region in value-based care and to ‘be a part of the solution.’ To help us grow and enhance our support for our providers, our employees, and – most importantly – our patients, DVACO has entered into an exciting and innovative partnership with Humana to expand upon those goals.
To facilitate our ability to thrive in the value-based world, we are thrilled to welcome Humana as the new partner in DVACO. As one of the nation’s leading health and well-being companies, Humana has deep expertise in managing population health; a proven track record of enhancing quality ratings and performance in value-based contracts; and access to best-in-class tools that will help us advance our value-based work. They, too, share our commitment to improved health outcomes and making quality care more affordable and accessible.
DVACO will continue to operate, as we always have, with a focus on providing high quality, high value, well-coordinated care and supporting the teams who make that care possible. Our dedication to our mission will not change. DVACO will remain a collaborative, multi-payer organization committed to the health and wellness of the Greater Philadelphia region. “
About Delaware Valley Accountable Care Organization (DVACO)
The Delaware Valley Accountable Care Organization (DVACO) is a limited liability company that is owned by Main Line Health and Jefferson Health, serving the Greater Philadelphia region. DVACO’s purpose is to enhance the quality of health care and reduce the growth rate of health care costs by acting as a convener, accelerator, and provider of the foundation needed to assist its participating members to transition from fee for service, a business model focused on volume, to a model focused on population health.
DVACO operates under the Medicare Shared Savings Program (MSSP) through an agreement with the Centers for Medicare and Medicaid Services (CMS). Currently, DVACO is the region’s largest Medicare ACO with more than 2,000 physicians and 90,000 Medicare fee-for-service beneficiaries. Additionally, DVACO currently holds multiple performance-based contracts with private payers as well as the employees and dependents of its owners—enhancing DVACO’s total number of beneficiaries to above 250,000.
About Main Line Health
Founded in 1985, Main Line Health is a not-for-profit health system serving Philadelphia and its western suburbs. Main Line Health’s commitment—to deliver advanced medicine for treating and curing disease, playing an important role in prevention and disease management as well as training physicians and other health care providers—reflects our intent to be the region’s premier choice for clinical care, research, and education. A team of more than 10,000 employees, 3,000 nurses and 2,000 physicians care for patients throughout the Main Line Health System.
At Main Line Health’s core are four of the region’s most respected acute care hospitals—Lankenau Medical Center, Bryn Mawr Hospital, Paoli Hospital and Riddle Hospital—as well as one of the nation’s premier facilities for rehabilitative medicine, Bryn Mawr Rehabilitation Hospital.
Main Line Health also includes Mirmont Treatment Center for drug and alcohol recovery; Main Line Health HomeCare & Hospice, which includes skilled home health care, hospice and home infusion services; Main Line Health Centers, primary and specialty care, lab and radiology, and other outpatient services located in Broomall, Collegeville, Concordville, Exton, King of Prussia and Newtown Square; Lankenau Institute for Medical Research, a biomedical research organization; and Main Line HealthCare, one of the region’s largest multispecialty physician networks.
Main Line Health is the recipient of numerous awards for quality care, and service, including U.S. News & World Report’s Best Hospitals, System Magnet® designation; the nation’s highest distinction for nursing excellence and the Mid-Atlantic Alliance for Performance Excellence (MAAPE) Excellence Award. Main Line Health is committed to creating an environment of diversity, respect, equity, and inclusion, has proudly received awards in this area and has embraced the American Hospital Association’s #123forEquity Pledge to Act to eliminate disparities in care. We are dedicated to advancing patient-centered care, education, and research to help patients stay healthy and live their best lives.
About Jefferson
Jefferson, located in the greater Philadelphia region and southern New Jersey, is reimagining health care and education to create unparalleled value. Jefferson is more than 40,000 people strong, dedicated to providing the highest-quality, compassionate clinical care for patients, preparing tomorrow’s professional leaders for 21st century careers, and discovering new treatments to define the future of care. Thomas Jefferson University, home of Sidney Kimmel Medical College, dates back to 1824 and today comprises 10 colleges and four schools offering 160 undergraduate and graduate programs to more than 8,200 students. Jefferson Health serves patients through millions of encounters each year at 18 hospitals (10 are Magnet® designated by the ANCC for nursing excellence) and over 50 outpatient and urgent care locations throughout the region.
About Humana
Humana Inc. is committed to helping our millions of medical and specialty members achieve their best health. Our successful history in care delivery and health plan administration is helping us create a new kind of integrated care with the power to improve health and well-being and lower costs. Our efforts are leading to a better quality of life for people with Medicare, families, individuals, military service personnel, and communities at-large.
To accomplish that, we support physicians and other health care professionals as they work to deliver the right care in the right place for their patients, our members. Our range of clinical capabilities, resources and tools – such as in-home care, behavioral health, pharmacy services, data analytics, and wellness solutions – combine to produce a simplified experience with the goal of making health care easier to navigate and more effective.
More information regarding Humana is available to investors via the Investor Relations page of the company’s website at humana.com, including copies of:
- Annual reports to stockholders
- Securities and Exchange Commission filings
- Most recent investor conference presentations
- Quarterly earnings news releases and conference calls
- Calendar of events
- Corporate Governance information.
###

